When a herniated or bulging disc in the neck is removed from the spinal column, a cervical fusion can be performed to replace it with a piece of bone taken from the pelvis or a bone graft from a bone bank. Normally, the bone graft fuses with the vertebrae above and below it. In some cases, however, this fusion does not occur. This is called Pseudarthrosis, a term that describes a failed fusion after spinal fusion surgery. This lack of fusion of the bones typically leads to abnormal movement of the bones within the spinal column. Pseudarthrosis may also describe the fracture of a bone that fails to heal or fuse together properly. Pseudarthrosis is a common complication of cervical spinal fusion surgery.
Pseudarthrosis occurs when bones fail to fuse with one another after spinal fusion surgery. Factors that reduce the ability of bone-producing cells (called osteoblasts) to produce new bone for fusion increase the risk of Pseudarthrosis. The most common contributor to Pseudarthrosis is smoking, as nicotine seems to block the ability of the osteoblasts to form new bone. Other factors that increase the risk of Pseudarthrosis are malnutrition, obesity, osteoporosis, diabetes, and rheumatoid arthritis. People who use oral steroids or non-steroidal anti-inflammatory medications are also at higher risk. The elderly are more likely to develop Pseudarthrosis as well as those who do not allow enough recovery time following fusion surgery. Too much activity will prevent the bones from fusing properly.
The most common symptom of Pseudarthrosis after cervical fusion surgery is neck pain, although some people exhibit no symptoms. The neck pain may be aggravated by moving the neck, and it can radiate into the shoulder or arm.
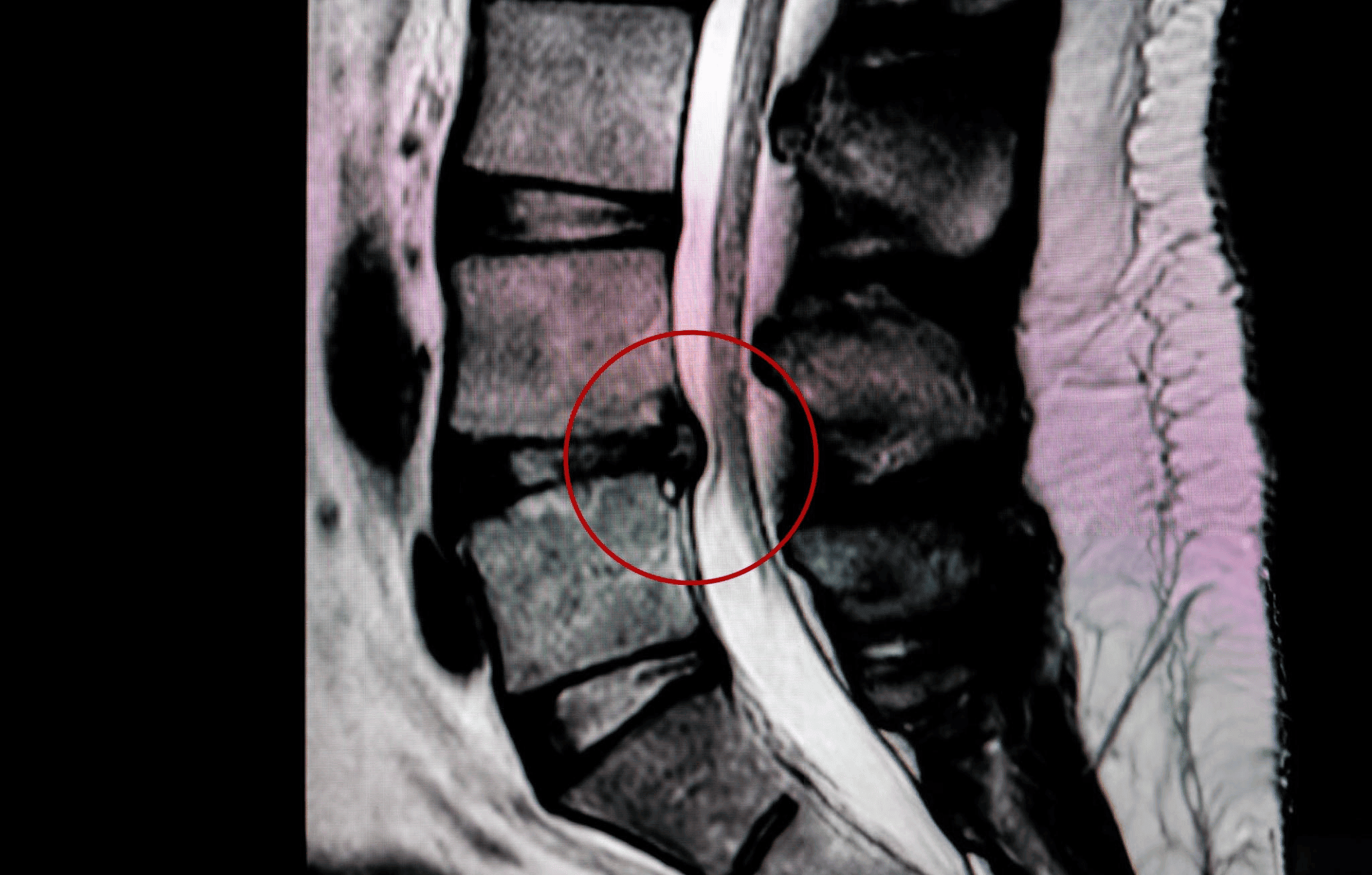
The diagnosis of Pseudarthrosis can sometimes be made using neck X-rays, including flexion and extension X-rays. Flexion and extension neck X-rays are taken with the neck in both a flexed and an extended position. This dynamic type of x-ray is more likely to show abnormal movement at the site of the fusion. In some cases, more advanced imaging studies such as nuclear medicine bone scans, CT scans, MRI scans, or surgical exploration may be needed before making the diagnosis.
In the absence of significant symptoms, surgery may not be necessary. For those who do have symptoms, a repeat fusion may be needed to give the bones a second chance to heal and fuse properly. Using additional hardware such as titanium plates may add the required support and stabilization. Surgery can be offered both anteriorly or posteriorly.